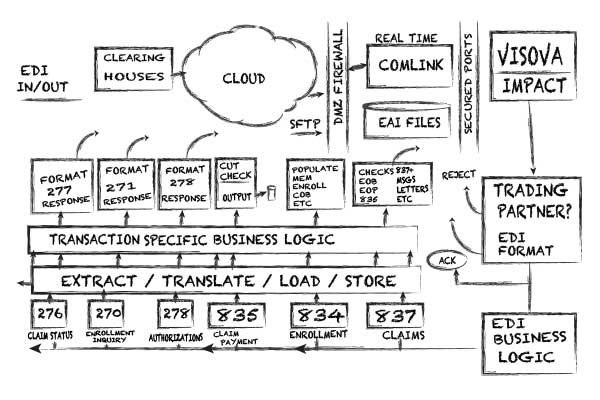
MCSI has vast experience with standard and non-standard EDI transactions.
EXPERIENCE
- Real-Time or Batch
- Inbound/Outbound and Complex Client driven Chaining
- Data Scrubbing
- Hierarchical Search Rules
- Trading Partner and Format Management
- Rejections and Acknowledgements
ELECTRONIC DATA EXCHANGES:
- Enrollment data and verification
- Claims submission (Medical, Dental, Pharmacy, etc.)
- Accumulator information
- Payment remittance advice
- Transaction acceptance
- Referrals and authorization
- Premium payments
- ACH/Credit card transactions
- Provider Network Rosters
HIPAA EDI TRANSACTIONS :
- 270 - Eligibility Request
- 271 - Eligibility Response
- 276 - Claim Status Request
- 277 - Claim Status Response
- 278 - Claim Review Request
- 278 - Claim Review Response
- 834 – Enrollment
- 835 - Claim Payment
- 837 - Professional Claim
- 837 - Dental Claim
- 837 - Institutional Claim
- 997/999 - Acknowledgement